 Accordingly, it contributes to the classical concept physiological dead space. Therefore, a right-to-left shunt widens the difference between alveolar carbon dioxide tension (PaCO 2) and PaCO 2, which defines the alveolar dead space (see Equation 1, below). Venous blood has a higher carbon dioxide content than does arterialized blood from ventilated and perfused lung units, and a shunt thereby leads to an increase in arterial carbon dioxide tension (PaCO 2). Part of venous blood thereby passes the lung without exchanging carbon dioxide and then mixes with arterial blood. In ARDS intrapulmonary shunt depends on collapsed lung units that are perfused but not ventilated. In a ground breaking study, West showed that this impedes gas exchange by increasing alveolar dead space. Other compartments may have a broad distribution of ventilation/perfusion relationships. 
Ventilated compartments with nearly zero perfusion may result from microthrombosis. In a complex relationship, dead space at the alveolar level reflects uneven ventilation/perfusion among lung compartments.  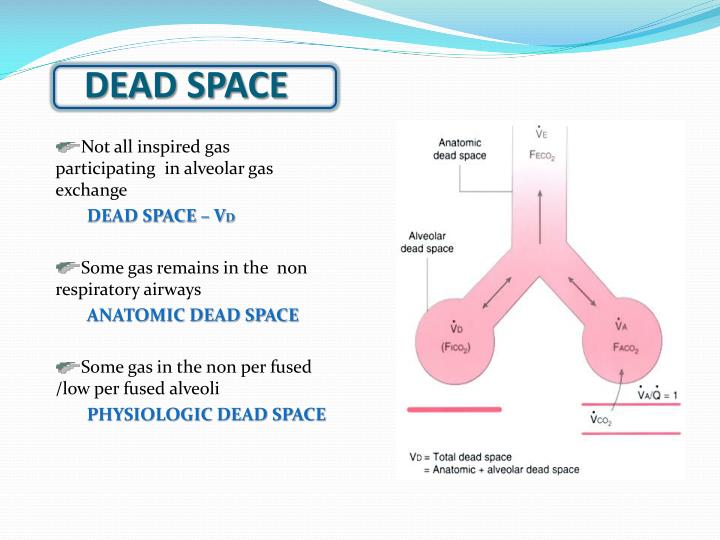
Airway dead space is increased by connecting tubes, often including a humidifying filter, and by limiting time for equilibration between airway and alveolar space. This impedes gas exchange and efforts to ventilate at low tidal volume in order to provide lung protective ventilation. In acute respiratory distress syndrome (ARDS), dead space is often high. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
